The Power of Egg Freezing for Future Family Planning

Egg freezing or oocyte cryopreservation removes some of the stress from family planning and allows you and your partner to decide the right time for a baby. The reasons a female may opt for egg freezing vary. In the case of a cancer patient undergoing treatment that threatens their ovarian reserve or reproductive system egg […]
Learn How to Use a Fertility Calculator

Fertility and conception rely on timing. For those females with regular or “normal” menstrual cycles, ovulation typically occurs mid-cycle. For example, if there are 30 days between periods, you may estimate ovulation at 16 days after the start of your period. A 28 day cycle may indicate ovulation occurs at 14 days, and so on. […]
How Tubal Reversal Works: Candidates & Options
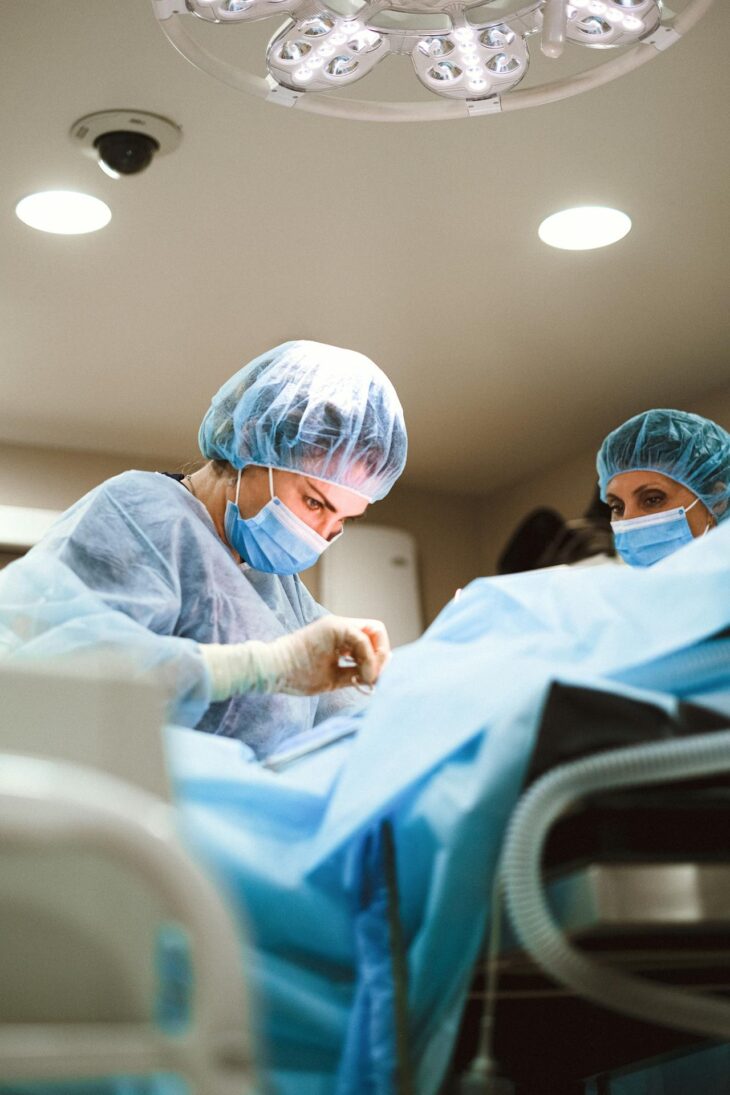
A tube reversal is the procedure that reverses tubal ligation. A tubal ligation, also known as having your tubes “tied”, provides a permanent form of birth control for females. Sometimes those who’ve had a tubal ligation decide, for myriad reasons, do, in fact, wish to conceive at a later date. When this occurs, many females […]
What You Can Learn About Infertility with Genetic Screening

Today doctors routinely suggest genetic screening to couples as part of their pre-pregnancy counseling. These tests screen both partners for more than 100 diseases and conditions. The conditions may impact your fertility, cause potential loss of future pregnancy by increasing your risk for miscarriage, or pose a threat of birth defects in your future child. […]
Egg Freezing 101: What Couples Should Know

An increase in maternal age, not finding the right partner yet, health concerns and a whole lot of other personal reasons lead couples and individuals to egg freezing. Freezing your eggs is an opportunity afforded to females by modern technology and means that biological clock may not tick quite as loudly as before. However, there […]
How to Know It’s Time to Seek Professional Fertility Guidance

When you’re trying to conceive and it just isn’t happening you may question your fertility. And as you consider the future fate of your ability to conceive you may wonder if it’s time you and your partner seek professional fertility guidance. According to the American College of Obstetricians and Gynecologists, experts recommend an infertility evaluation […]
Can Uterine Fibroids Affect Fertility?

Uterine fibroids are very common among females of childbearing age, affecting 35%-77% according to the NIH. They are nearly always benign or non-cancerous, and many women have no recognizable symptoms alerting them to fibroids. Uterine fibroids don’t increase the risk for cancer of the uterus and for the most part uterine fibroids don’t have an […]
5 Common Infertility Testing Questions, Answered
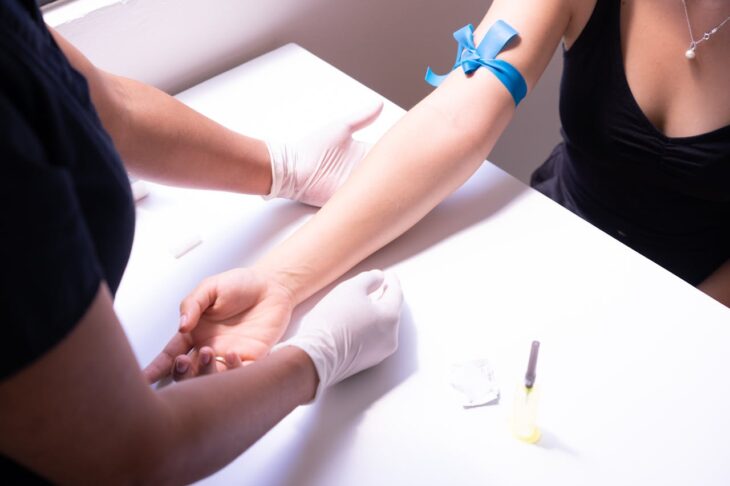
For most couples it takes up to a year of unprotected intercourse to conceive. If you and your partner have had no success and each month brings disappointment, you may wonder if you’re infertile. Often couples experience no symptoms of infertility other than an inability to conceive after many months of trying. Your Infertility […]
Endometriosis: Signs & Fertility Implications

People generally recognize endometriosis as a painful and somewhat debilitating condition. Endometriosis often causes heavy bleeding and intense cramping in females of childbearing age. There are also other symptoms but it may surprise you that around 25% of those females who suffer the condition are asymptomatic, meaning they have no identifiable symptoms. Most couples receive […]
Acupuncture & Fertility: 5 Things to Know

Acupuncture is the practice of inserting very fine needles into the body at certain points. There are certain points located along the meridians, or energy channels, which when manipulated may correct imbalances within the body. Acupuncture is a key component in the practice of Traditional Chinese Medicine and restores homeostasis, or optimal function, to the […]
